Real solutions for Rhode Islanders
As a local, nonprofit health insurer, Blue Cross & Blue Shield of Rhode Island (BCBSRI) took innovative, collaborative approaches to helping our members and our neighbors navigate a challenging year in healthcare. Here's a look at the progress we made together.
Measuring what matters
At BCBSRI, we serve our mission and our members, not shareholders. These outcomes show our focus on improving the health of Rhode Islanders and reducing the high cost of healthcare.
200,000+
youth connected with mental health support and prevention
9,250+
free health assessments conducted with members to identify care needs
50,000+
care management services delivered to our members
$43M
saved by avoiding added growth in healthcare costs, including through improved pricing and enhanced support for serious health conditions
$20M
saved in operating expenses, including through technological efficiencies and consolidated vendor contracts
94%
of businesses chose to renew their employees' BCBSRI coverage
346,860+
neighbors impacted by our investments in housing, food security, and other community programs
9,480+
hours volunteered by BCBSRI associates
137,120+
visits to our stores and community events
Real solutions for expanding access to quality care
Better health and lower costs can go hand in hand. From primary care offices to local schools, we connected our members and our community with high-quality, cost-effective care.
Strengthening primary care in our state
By helping prevent and manage chronic conditions, primary care providers (PCPs) are essential for protecting our members’ health and managing overall healthcare costs. In 2025, we took significant steps to support primary care in our state:
- Increased payments to PCPs for our fully insured commercial plans by 35%, as mandated by the Office of the Health Commissioner’s updated affordability standards. Rhode Island PCP rates are now on par with Massachusetts. We’ll make additional rate increases totaling more than 50% by 2028.
- Voluntarily eliminated most primary care medical prior authorizations, which can reduce the administrative burden for PCPs.
- Introduced a contracting option that pays PCPs a fixed amount each month to improve their financial stability. This helps PCPs expand their care team, which increases access for our members.
Alongside these efforts, we acted quickly to help our members when one of the state’s largest primary care practices closed with short notice last year. We coordinated with primary care practices that had the capacity to accept new patients and contacted 100% of our impacted members—95% chose a new PCP. We secured 7,000+ new patient visits for members who lost their PCPs.

$500+ million
invested by BCBSRI in primary care—beyond the rates we pay doctors—over a 10-year period to help increase access to preventive and team-based care, including visits with nurses and pharmacists.
Alongside these efforts, we acted quickly to help our members when one of the state’s largest primary care practices closed with short notice last year. We coordinated with primary care practices that had the capacity to accept new patients and contacted 100% of our impacted members—95% chose a new PCP. We secured 7,000+ new patient visits for members who lost their PCPs.

Reaching more than half of RI youth with mental health support
After the pandemic, many of our children were struggling. We set a goal to support half of the state’s youth—110,000 kids and teens—by 2025. Together with our community partners across the state, we worked to expand preventive efforts, with programs in nearly every school district in the state. We exceeded our goal and are seeing encouraging progress—reaching over 200,000 kids and teens. For our members, we also increased access to care and supported integration of behavioral health into primary care, resulting in lower hospital admissions and emergency room visits.
200,000+ youth
connected with mental health support and prevention from 2023-2025
Real solutions for delivering personalized support
House calls. Virtual visits. Digital wellness tools. All at no extra cost to our members. By meeting members where they are, we’re helping them improve their health and reduce avoidable ER visits and hospitalizations.
Offering 24/7 help to members living with cancer
The members in our new cancer care support program consistently tell us their healthcare experience now feels more coordinated, more personal, and less overwhelming. The program, launched in collaboration with Daymark Health1, was designed in partnership with local cancer institutes to provide additional support to our members to help them navigate oncology care. With deep experience in cancer care, Daymark works closely with members’ doctors to support their treatment plan.
- At-home & virtual visits
- Around-the-clock support and regular check-ins
- Assistance with scheduling timely appointments
- Help accessing the best care close to home for comfort and convenience

89 Net Promoter Score
for our cancer care support program, indicating a world-class level of customer satisfaction and loyalty
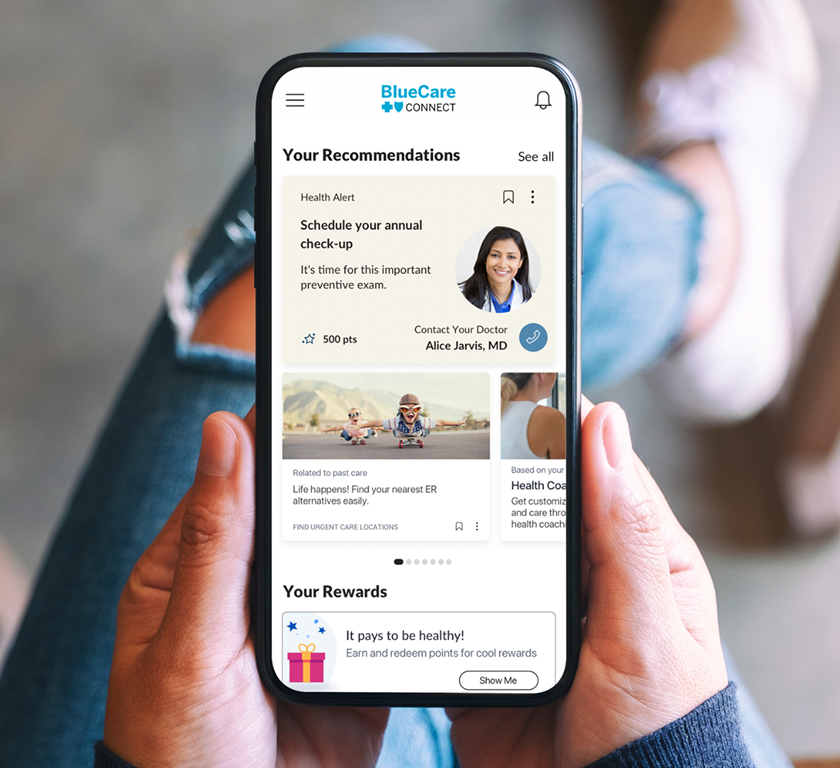
Helping members make the most of their healthcare
To make it easier for our members to navigate the complex healthcare system, we introduced BlueCare Connect in 2025. Available online, through our app, or over the phone, BlueCare Connect brings together all of our members’ health benefits in one convenient location. Our members can access wellness programs, coverage information, chronic condition support, and customer service—and get personalized health support from Care Guides, nurses, and coaches.
A member wanted to improve her nutrition and be more active, so I helped her set goals and connected her with resources. After four months, she met 99% of her goals and was really excited about her progress.
Michelle, RN, BlueCare Connect health coach
14,000+
calls where Care Guides provided additional support, from reminding members about screenings to connecting them with health programs
67,000+
members registered for the BlueCare Connect app
Connecting more members with extra care
For our members living with chronic health conditions, extra help can improve their health and their lives. We offer tools and support to help members get the care they need and reduce their risk for complications, including hospital care.
We offer personalized programs for the most common health challenges our members face. In addition to our cancer care support program, we introduced new programs for members living with kidney disease and made remote monitoring devices available to members with congestive heart failure and chronic obstructive pulmonary disorder. We also made existing programs more widely available.
18,290+
visits through HouseCall by Blue, which was expanded to include all eligible members
9,250+
health assessments in homes, through telemedicine, and (new in 2025) in Your Blue Store℠ and on Your Blue Bus
50,000+
care management services delivered to our members
Making it easier to get cancer screenings
From partnering with community organizations to drop off home test kits to arranging transportation for colonoscopies, we continued our campaign to increase screenings for colorectal cancer, which is highly preventable and treatable when caught early. We also sent email and text reminders to more than 25,000 members who were overdue for screenings for cancer and other diseases.

50%
reduction in racial disparities in colorectal screenings since 2022
10.7%
increase in overall colorectal cancer screening rates since 2022
Real solutions for improving the health of our neighbors
Serving our community is at the heart of everything we do. In 2025, we supported more than 200 local nonprofits that are working to make life better for Rhode Islanders.
Understanding the challenges facing our community
To prioritize how we can best help our neighbors, we listen to them by turning to the RI Life Index. This statewide survey, a partnership of BCBSRI and the Brown University School of Public Health, provides a detailed snapshot of how our neighbors perceive the factors affecting their well-being. The overall score of 57 (on a 1-100 scale) was unchanged from 2024, the lowest score recorded.
In 2025, a companion to the RI Life Index, RI Voices, provided a deeper understanding of the urgent issues affecting Rhode Islanders, including housing and food security.



Responding to a crisis in food assistance
Over the last five years, an increasing number of our neighbors have needed help putting healthy food on the table. We support—and deeply value—the work of local nonprofits that are helping fill the plates of Rhode Islanders. In 2025, with rising prices, the federal government shutdown, and a lapse in SNAP benefits, the need for food assistance was record-breaking. In response, we gave emergency grants in appreciation of the dedicated staff at 15 agencies doing vital work to address food access.
87,300+
neighbors impacted by our food security investments
Highlighted programs
We're proud to support these nonprofits and many others addressing food security in our state.

RI Community Food Bank
Distributing food through their network of member agencies across the state

Farm Fresh Rhode Island
Increasing healthy food access for women, children, and seniors

The ELISHA Project
Providing food and household essentials through pop-up share markets
Supporting access to affordable housing
Having a safe, affordable place to live is important for the well-being of every Rhode Islander. Through our 2025 BlueAngel Community Health Grants and individual project funding, we continued to invest in nonprofits helping our neighbors access stable housing—from creating new apartments to arranging rental assistance to providing legal services.
13,500+
neighbors impacted by our housing investments

Showing up as 1 Blue 4 RI
Our favorite day of the year is Blue across Rhode Island, our annual day of service. To celebrate our 14th year, we rolled up our sleeves to volunteer for 14 local nonprofits.
560+
volunteers
3,000+
volunteer hours
33,300+
Rhode Islanders impacted

BCBSRI was honored to be named one of America's 50 most community-minded companies by Points of Light—the world's largest organization dedicated to volunteer service.
Companies like Blue Cross & Blue Shield of Rhode Island are leading the way in showing how social impact benefits their employees' well-being, strengthens the communities where they do business, and brings value and meaning to their work.
Jennifer Sirangelo, President and CEO, Points of Light
Working together to bring healthcare costs under control
At BCBSRI, we know that rising healthcare costs are a real concern for families, businesses, and our state—and deserve real solutions.
In 2025, healthcare costs continued to rise at unprecedented levels. We saw increases in every category of care and in every market we serve, which drove up premium costs.
The financial pressure facing our members and customers is significant—and unsustainable. To help control healthcare costs, we took action to tackle the root causes driving these increases, working in collaboration with our provider partners and the community. We also lowered our operating expenses to achieve additional savings on behalf of our members.
We must continue to work together to create the healthcare system that Rhode Islanders deserve.
Managing costs with high-quality, cost-effective care
In 2025, the amount BCBSRI spent on medical and pharmacy claims increased by $183 million from 2024. To help reduce the impact of rising costs on families and businesses, we worked throughout the year to negotiate better pricing and improve the quality of care for our members, leading to $43 million in savings from avoided costs. As part of these efforts, we helped make medicines more affordable. We also provided extra support to help members with serious conditions improve their health and avoid unnecessary hospital care.

$43 million saved
by avoiding added growth in healthcare costs in 2025

Lowering operating expenses
In 2025, BCBSRI consolidated vendor contracts, deployed technologies for greater efficiency, and reduced our workforce with a focus on leadership roles. While administrative costs are a small percentage of total costs, we're working to lower them further.
$20 million saved
in operating expenses in 2025
Addressing drug costs through negotiated pricing and innovation
We're focused on strategies that help members get the medication they need at a cost they can afford, including:
- Partnering with Blue Cross Blue Shield companies to collectively negotiate lower prices on high-cost specialty drugs through Synergie Medication Collaborative2 and to manufacture lower cost generic medications through CivicaScript3
- Shifting to biosimilar and generic medications that offer comparable quality at significantly lower costs
- Working with local health systems to deliver specialty drugs, which saves money, helps patients get drugs faster, and provides crucial revenue to local providers
Our CEO’s perspective
Our President & CEO Martha L. Wofford shares creative, collaborative approaches for controlling healthcare costs and improving access to high-quality, affordable care.
Please note that you may need a Boston Globe subscription to access the article.
BCBSRI saw healthcare costs rise in every area of care in 20254
14%
driven by increased high-cost hospital admissions
8%
driven by increased visits to specialists and other providers and increased reimbursement for PCP visits
7%
driven by specialty drugs and GLP‑1s for diabetes
6%
driven by increased costs for outpatient procedures
Improving stability in a challenging environment
In 2025, medical and pharmacy costs continued to rise at unprecedented levels both nationally and locally, pushing healthcare premiums to unaffordable levels. At BCBSRI, we took important steps to improve management of medical costs and lower administrative expenses, reducing our operating losses by $37 million from 2024.
While we improved business fundamentals, we experienced a $78 million operating loss on a normalized basis*, requiring ongoing diligence to restore the company to break-even financial performance and to make healthcare more affordable.
Normalized operating results give a clearer view of our underlying performance, removing one-time adjustments and items related to other years. With those adjustments and items included—and with the benefit of investment income—we ended the year with a net gain of $14 million on a reported basis.
As a local, tax-paying nonprofit health plan, we serve our members and not shareholders. Any money remaining after paying claims and expenses goes into a reserve fund for the future protection of our members.
There is significant work to be done to continue to reduce healthcare costs, and it must be done in collaboration with our provider and community partners to ensure the sustainability of our healthcare system for our members, customers, and all Rhode Islanders.
Reported financial results
These numbers reflect reported results.
$2.43 billion
In 2025, we recorded nearly $2.43 billion in premiums from members (individuals and employers).
$2.44 billion
From total revenue, more than $2.19 billion was used for medical and dental claims for our members. This amount accounted for 90.4% of premium revenue collected. The organization spent more than $267 million, or 10.8% of premiums (including premium taxes), on expenses to support the core operations of our business.
$10 million
Our premium revenue didn’t cover our total expenses, resulting in an operating loss of $10 million. (On a normalized basis, the operating loss was $78 million as described above.)
$24 million
We recorded a $24 million gain from investment income.
$14 million
Overall, total revenue stood at more than $2.45 billion, and expenses were nearly $2.44 billion in 2025, resulting in a net gain of $14 million.
$362 million
In 2025, statutory reserves that we held for the protection of our members totaled more than $362 million at year-end. This reflects an increase of $25 million from the previous year. This is money we set aside to pay future claims and equals about 2 months of claims paid.
*Normalized results should be considered in conjunction with, not as a substitute for, reported financial results.
NOTE: Numbers may not add up due to rounding. This formulation represents unaudited results utilizing Statutory Accounting Principles. The Blue Cross and Blue Shield Association licenses Blue Cross & Blue Shield of Rhode Island to offer certain products and services under the Blue Cross and Blue Shield brand names. Blue Cross & Blue Shield of Rhode Island is an independent organization governed by its own Board of Directors and solely responsible for its own debts and other obligations. Neither the Association nor any other organization using the Blue Cross and Blue Shield brand names acts as a guarantor of Blue Cross & Blue Shield of Rhode Island's obligations. A copy of Blue Cross & Blue Shield of Rhode Island's most recent financial statements is available at the state Department of Business Regulation.
1Daymark Health, Inc. (“Daymark”) is an independent company contracted with BCBSRI to provide care coordination services. Daymark has contracted with Daymark Health DE LLC (“Medical Group”) to enable access to Medical Group’s employed licensed providers to provide clinical services.
2Synergie Medication Collective℠ is an independent entity owned by a group of Blue Cross and Blue Shield affiliated companies.
3Civica Rx is an independent company partnering with Blue Cross & Blue Shield of Rhode Island and other Blue Cross and Blue Shield companies to provide select generic drugs to members.
4The increases noted are for fully insured BCBSRI commercial plans.







